Building the infrastructure for Food as Medicine to thrive
The purpose of NVP is to codify, operationalize, and expand FAM benefits by building scalable infrastructure, shared referral pathways, and implementation tools that support integration across healthcare systems, payers, and food providers.
Systems mapping of FAM programs, stakeholders, and workflows across Michigan
Pilot program implementation across health care quality improvement initiatives including oncology, diabetes, and surgical care
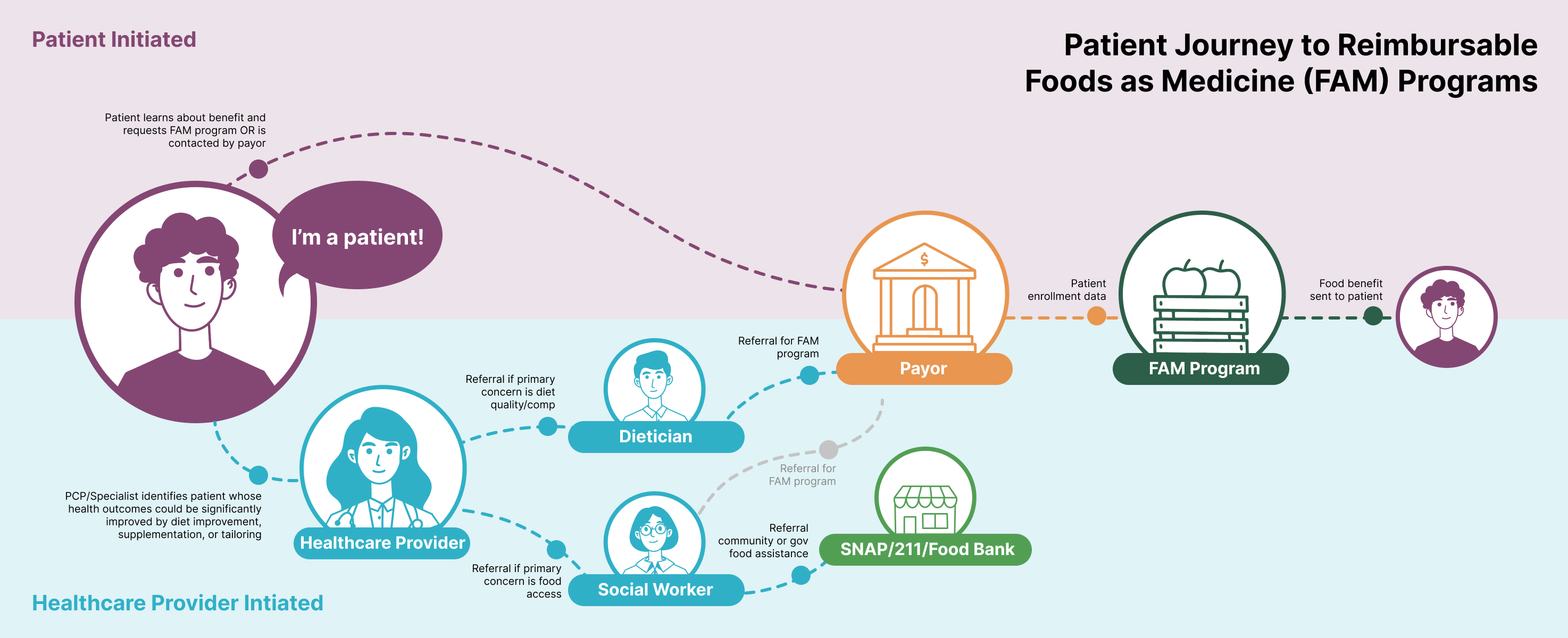
Development of referral workflows for both patient-initiated and provider-initiated pathways
Centralized ILOS/FAM benefit information hub and digital navigator
Toolkits and resources to support providers, payers, and patients across the state
Development and dissemination of a replicable roadmap for successful FAM implementation
Definition Food as Medicine (FAM)
Medically appropriate nutrition interventions to prevent, manage, or treat disease. Examples including medically tailored meals, healthy food packs, and produce vouchers for conditions like diabetes or cancer.
Definition In Lieu of Services (ILOS)
In Michigan, ILOS allows Medicaid health plans to optionally offer FAM benefits to address members’ nutrition-related health needs. These benefits are funded by the health plans themselves as lower-cost alternatives to more expensive medical care.
Definition Food Vendor / Provider
An organization supplying healthy food or meals as part of FAM programs. Examples: Mom’s Meals (statewide medically-tailored delivered meals) and The Farm at Trinity Health (locally grown produce for healthy food packs in southeast Michigan).
ResourceFAM 1-Pager
Want to learn more or share information? Download our 1-pager on FAM programs in the state of michigan!
Download PDFOur VisionA healthcare future where food is foundational. Nutrition policy becomes practice, and practice yields value to patients, clinicians, communities, and health care systems. Food benefits are scalable, sustainable, with clear pathways to access and utilization.
The NVP is activily meeting with leaders across this system to support collaboration and knowledging sharing between stakeholders.
.png)

Medical teams are stretched thin. At the same time, accessing real food resources can feel like a superpower or ray of hope. Clinicians need clear and simple referral protocols, accurate program info, and direct-to-patient support from programs.

The health of our communities depends on the work of local farms, grocery stores, meal delivery providers, and food security organizations. These groups are motivated to get food to patients and to work with health and policy partners to drive value.

90% of U.S. health costs relate to chronic diseases. How do we get a handle on it?
Payors want better patient outcomes, happier members, and lower health care costs.

Food as medicine has captured the attention of the nation. Health policies that strengthen healthy food access meet the strategic moment and compliment existing food programs. But what do food benefits look like in practice and how can we measure success?

a Collaborative Quality Initiative (CQI) transforming healthcare through design.
